Sadly, eye injections came too late for Joyce Chamberlain. But thousands of Australian patients will now be able to stick to this sight-saving treatment after both major political parties rejected a proposed Medicare rebate cut.
Joyce Chamberlain loved to knit.
But when the Wodonga pensioner developed neovascular age-related macular degeneration (wet AMD) in her early 60s, blindness forced her to hang up her knitting needles.
“Once her eyesight went, that was the end of it,” Joyce’s daughter Cheryl recalls of her late mother.
“That was really hard for her because she used to sit up night after night, making dresses for us when we were kids.
“When grandchildren come along, she knitted their booties and jackets and sleeping bags, all that sort of stuff. Then that all went by the wayside.”
Breakthrough treatment
When Joyce was diagnosed with wet AMD in the early 1990s, no treatment was available, and she lived with no central vision in both eyes for the last three decades of her life.
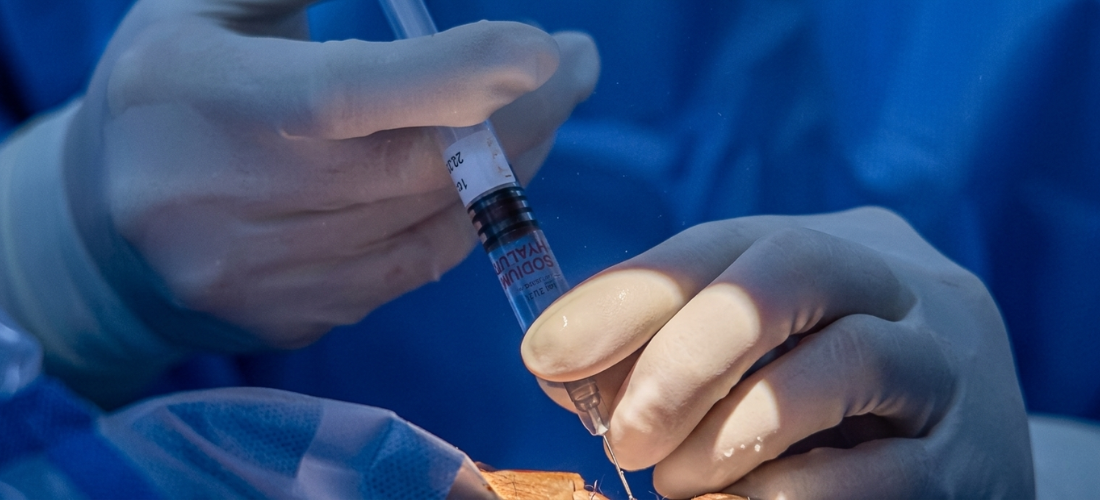
Sight-saving eye injections eventually arrived in Australia in 2007, but this major breakthrough came too late for Joyce and countless others.
When treatment became available 15 years ago, Joyce received injections to cling onto whatever vision was left, “but it didn’t matter anyway because she’d already lost her sight,” Cheryl says.
“It was already gone – it was gone within six months of being diagnosed.”
For people diagnosed after 2007, their outlook is very different.
Australia is a world leader in the treatment of wet AMD. Eye injections have saved the sight of thousands of Aussies, who can now enjoy full, active lives long after diagnosis.
Barriers to treatment
However, about one in five patients drop out of treatment inside 12 months, and the majority give up within five years. Cost is the major barrier, with the average patient out of pocket $1900 a year – double if they need injections in both eyes.
Alarmingly, the independent Medicare Benefits Schedule Review Taskforce for Ophthalmology recommended a 69 per cent cut to the Medicare rebate for eye injections – a move that would have made this treatment even more expensive.
MDFA worked with both sides of politics and presented them with PwC economic modelling that calculated patients’ average out-of-pocket costs would more than double if this cut was made.
That extra financial burden threatened to lead 47,000 Australians to give up treatment over a five-year period – and when you give up injections, you risk going blind.
However, in the build-up to May’s Federal Election, both Labor and the Coalition committed to rejecting the recommended cut regardless of the Election result.
That decision represents a major win for thousands of macular disease patients who rely on this treatment to retain their sight.
“Hopefully better treatment is available”
Sadly, effective treatment for wet AMD came too late for Cheryl’s mother Joyce.
Cheryl’s family history means she carries a one-in-two chance of being diagnosed with AMD, which is why she diligently visits her optometrist every year for an eye exam, including a check of the macula.
Detecting any symptoms early, and beginning treatment quickly, are the keys to saving sight. Cheryl has her fingers crossed for even more breakthroughs in future.
Australian regulators are currently reviewing two new treatments that could ease both the physical and financial toll on patients.
“Hopefully, by the time something ever happens to me, better treatment is available,” Cheryl says.
“When your eyesight goes, that’s it – you can’t drive a car, you can’t get around, you’re virtually stuck in the house.”
Posted: 26 May 2022