Eye exams and early diagnosis of diabetic eye disease
Regular eye exams with your eye health professional are vital to diagnosing diabetic eye disease and reducing the risk of vision loss.
Eye exams can identify diabetic retinopathy (DR) at its earliest stage before vision loss has occurred.
If you have diabetes, you should have an eye exam when first diagnosed with diabetes. Follow-up eye exams are needed regularly – at least every two years.
Once you have been diagnosed with diabetic eye disease, you should have an eye exam at least once a year. Your eye health professional will advise you if you need to have eye exams more frequently.
When you see your eye health professional, it’s important to tell them that you have diabetes. They will also want to know how long you’ve had diabetes and your most recent HbA1c result. Your HbA1c result is a summary of the average blood sugar level over the past three months. You should also let your eye health professional know about any medications you’re taking.
Even if your eye exams have been normal in the past, you must continue having them regularly.
So, what happens when I have my eye exam?
An eye health professional will use several tests when diagnosing diabetic eye disease.
Vision testing
Vision testing – also called visual acuity testing – provides a measure of how well you see. This allows comparison of your vision with previous visits and is important for monitoring changes in vision over time.
Slit lamp retinal examination
Using a microscope-like instrument, your eye health professional will check the health of your eyes, including the retina, to check for signs of DR.
You may have your pupils dilated (enlarged) with eye drops, which allows a better view of the retina. The drops normally cause blurry vision and glare for a few hours. It’s unwise to drive while your vision is blurry, so arrange how to get home before your appointment. Sunglasses will help with glare while your pupils are dilated.
Supplementary testing
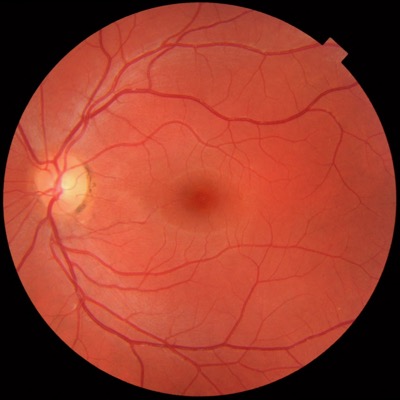
Retinal photography
One or more photographs of the retina are often taken of each eye to provide a detailed record of the level of diabetic retinopathy.
This can allow your eye health professional to make comparisons with your previous photographs. The rate of change in retinopathy over time can provide an indication of the risk of any sight-threatening changes. This is why retinal photography is a recommended part of your eye exam.
Ultra wide imaging allows a larger portion of the retina to be photographed. Because we know DR starts peripherally, ultrawide imaging is now preferred.
Optical coherence tomography (OCT)
This is a non-invasive imaging technique that uses light to produce very high resolution cross-sectional images of the layers of your retina. It’s particularly helpful to detect diabetic macular oedema, which appears as a collection of fluid within and under the retina.
Angiography
If you have leaking blood vessels or macular edema, your ophthalmologist may perform a fluorescein angiogram. Fluorescein is an orange dye that is injected into the blood via a vein in your arm.
This dye rapidly reaches the eye via the bloodstream and circulates through the retina.
A specialised camera, often with a blue-coloured flash, is used to take a series of images of the fluorescent dye as it passes through the blood vessels of the retina. This dye highlights areas of blood vessel leakage, abnormal blood vessels and areas of the retina that are not well supplied with blood.
This procedure only takes a few minutes.
Some OCT machines can perform a type of angiography (OCT-angiography) that doesn’t require dye injection.
Eye exam reminders
MDFA encourages everyone with diabetes to register with KeepSight. KeepSight is a national diabetic eye screening program, making it easier for people to schedule regular eye exams.







