What is diabetic retinopathy?
Diabetic retinopathy (DR) is a complication of diabetes. It is caused by damage to the small blood vessels in the retina, which is at the back of the eye.
Diabetic retinopathy is the leading cause of avoidable vision loss and blindness in working-age Australians.
Up to a third of Australians over the age of 50 living with diabetes have some evidence of DR.
Most people with diabetes will develop DR over time. However, the severity of disease is greatly influenced by how well your diabetes is controlled.
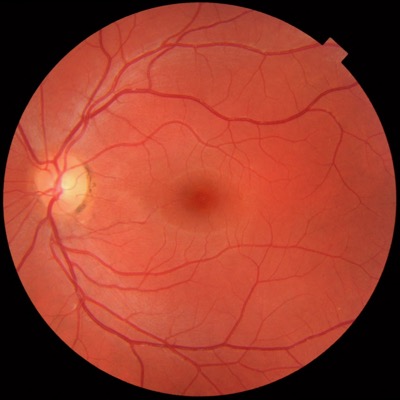

Non-proliferative diabetic retinopathy (NPDR)
NPDR occurs gradually when there is damage to the small blood vessels in the retina due to increased blood glucose levels.
The small, specialised blood vessels in the retina become weaker. They may also leak fluid and become blocked.
In the early stages, DR may not impact your vision. But you will need to see your optometrist or ophthalmologist every three to 12 months, depending on the severity of your disease.
Your eye health professional might suggest medication to slow disease progression.
As NPDR worsens, it may affect your vision. It could also progress to proliferative diabetic retinopathy.
Proliferative diabetic retinopathy (PDR)
PDR occurs when the reduced oxygen supply to the retina triggers the release of vascular endothelial growth factor (VEGF). This, in turn, stimulates the growth of new blood vessels (neovascularisation). These new fragile blood vessels tend to leak and bleed, affecting vision.
Scarring can also occur and as the scar contracts, the retina can detach.
If not treated early, PDR can result in blindness.
Diabetic macular oedema (DMO)
Diabetic macular oedema (also sometimes referred to as diabetic macular edema, or DME) can occur at any stage of the disease. It happens when leaking fluid from retinal blood vessels accumulates in the macula, the area of the retina that is specialised for detailed vision. This can cause the loss of detailed, central vision and even legal blindness.
Diabetic macular oedema requires treatment, either with injections to the eye or targeted laser treatment. The course of treatment will depend on on the individual circumstances, including how close the fluid leak is to the macula.




